The Hypoglycemia Problem Nobody Talks About With Retatrutide
Why the most powerful GLP-1 receptor agonist might be dropping your blood sugar—and what the research actually tells us
Disclaimer: This article discusses research compounds and is for educational purposes only. This is not medical advice. Consult qualified healthcare professionals before making any health decisions.
When I first started deep-diving into retatrutide research last year, I kept seeing the same pattern in community reports: people would be cruising along fine for a week or two, loving the appetite suppression and fat loss, then suddenly—wham—they’d be standing in front of their fridge at 2 AM, shaking, sweating, and shoveling whatever carbs they could find into their mouth.
Sound familiar?
If you’ve researched retatrutide (RT/Reta) and experienced this, you’re not crazy. And more importantly, there’s a clear scientific explanation for what’s happening—one that most people miss because they’re thinking about retatrutide like it’s “just a stronger semaglutide.”
It’s not. And that difference matters.
The Triple Threat That Changes Everything
Let’s start with the basics. Most people in the peptide research space are familiar with GLP-1 agonists:
Semaglutide (the active compound in Ozempic/Wegovy): GLP-1 agonist only
Tirzepatide (Mounjaro/Zepbound): GLP-1 + GIP dual agonist
Both work primarily by enhancing insulin secretion when you eat (keeping blood sugar stable) and suppressing appetite. Pretty straightforward.
Then there’s retatrutide: GLP-1 + GIP + GCGR triple agonist.
That third receptor—the glucagon receptor (GCGR)—is where things get interesting. And where the hypoglycemia risk comes from.
Understanding the GCGR Component
Here’s where it gets counterintuitive. In normal physiology, glucagon RAISES blood glucose. Your pancreas releases it when blood sugar drops, signaling your liver to release stored glucose. It’s your body’s anti-hypoglycemia hormone.
So why would a glucagon receptor agonist cause LOW blood sugar?
The answer lies in how GCGR activation works in the context of the other two pathways. When you activate all three receptors simultaneously:
GLP-1 activation: Increases insulin when you eat, suppresses glucagon release from pancreas
GIP activation: Enhances insulin response, shifts fat metabolism
GCGR activation: In this unique context, dramatically increases energy expenditure and fat oxidation
The result? Your metabolism shifts into overdrive. You’re burning fat faster, your muscles are taking up glucose more efficiently, and your overall energy expenditure increases. It’s metabolically powerful—which is exactly why retatrutide shows such impressive results in clinical trials.
But here’s the catch: your body now needs a baseline of glucose availability that it didn’t need before.
The Retatrutide Paradox
Think of it like this: you’ve just upgraded your car’s engine to burn fuel three times more efficiently. Great for performance—but now you need to actually keep fuel in the tank or you’re going to stall out on the highway.
This is what happens with retatrutide-induced hypoglycemia. You’re not eating “too little” in the traditional sense. You might be eating a reasonable amount of protein and fat. But your carbohydrate intake isn’t matching your new metabolic demands.
The research suggests that retatrutide creates what I call a “carbohydrate floor”—a minimum carb intake below which you risk crashing, regardless of total calorie intake.
The Warning Signs (And Why They’re Easy to Miss)
Here’s what makes retatrutide hypoglycemia tricky: the appetite suppression is so effective that you might not feel hungry even when your blood sugar is dropping.
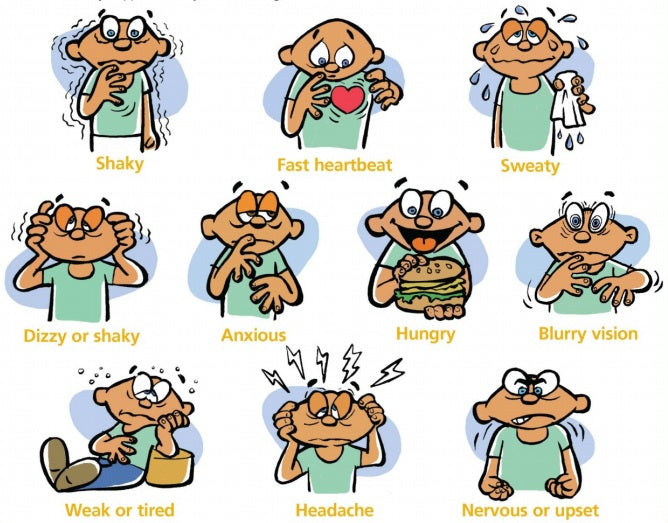
Watch for these signs:
Early Stage:
Sudden shakiness or trembling (especially in hands)
Cold sweats that come out of nowhere
Heart pounding or racing feeling
Mild dizziness or lightheadedness
Moderate Stage:
Difficulty concentrating or brain fog
Irritability or mood changes (the “hangry” feeling)
Extreme fatigue that hits suddenly
Visual changes (blurriness, tunnel vision)
Severe Stage:
Confusion or disorientation
Difficulty speaking clearly
Loss of coordination
In extreme cases: seizures or loss of consciousness
The dangerous part? Because retatrutide suppresses appetite so effectively, you might not get that urgent “I NEED FOOD NOW” signal until you’re already in moderate hypoglycemia.
What the Clinical Data Actually Shows
The phase 2 clinical trials for retatrutide reported hypoglycemia events, but here’s what they don’t tell you in the abstracts: most participants were on controlled diets with regular meal timing and macronutrient targets.
In the real world of research? People are intermittent fasting. Doing extended fasted cardio. Eating ketogenic diets. Stacking with other compounds. All things that compound the hypoglycemia risk.
The Eli Lilly trials used careful dose escalation:
Week 1-4: 0.5-1mg
Week 5-8: 2-4mg
Week 9-12: 4-8mg
Week 13+: 8-12mg
Why so slow? Because your metabolism needs time to adapt to each new level of receptor activation. Skip ahead too fast, and you’re asking for trouble.
The Prevention Protocol (Based on Research)
After analyzing the available research and community reports, here’s what actually works:
1. Respect the Titration Schedule
I know, I know—you want results faster. But jumping from 2mg to 8mg because “you’re not feeling anything” is how you end up face-down in a bowl of Lucky Charms at 3 AM.
Start low. Increase slowly. Give your body 4 weeks minimum at each dose level.
2. Strategic Carbohydrate Timing
This isn’t about eating massive amounts of carbs. It’s about strategic placement:
Morning: 20-30g carbs within 2 hours of waking (even if not hungry)
Pre-activity: 15-25g carbs before exercise or physical work
Evening: 30-50g carbs with dinner
Total daily might only be 80-120g, but the TIMING prevents crashes.
3. Recognize Your Personal Threshold
Everyone’s carbohydrate floor is different. Some people can research retatrutide on 50g carbs/day. Others need 150g+.
Track your intake for a week and note when symptoms occur. That’s your threshold. Stay above it.
4. The Fast-Acting Carb Kit
Keep these accessible at all times:
Glucose tablets (15g serving)
Small juice boxes (15-20g carbs)
Honey packets
Dried fruit
If you feel symptoms coming on: 15g fast carbs, wait 15 minutes, reassess. Don’t guess—measure.
5. Avoid Compounding Factors
These multiply hypoglycemia risk:
Fasted cardio: Especially HIIT or long duration
Alcohol: Impairs liver glucose production for hours
Meal skipping: Even if not hungry, don’t go >6 hours without eating
Other compounds: Especially those affecting insulin sensitivity
6. Monitor and Adjust
If you’re experiencing hypoglycemia more than once a week, something’s wrong:
Dose might be too high
Carb intake might be too low
Titration might have been too aggressive
Activity level might have increased without adjusting nutrition
Fix the variable. Don’t just “push through it.”
The Realities Nobody Mentions
Here’s what I wish someone had told me when I started researching retatrutide:
Reality #1: The appetite suppression is SO effective that you can easily under-eat carbs without realizing it. You’ll feel “fine” eating just protein and fat—until suddenly you’re not fine.
Reality #2: Hypoglycemia episodes can create a psychological relationship with food that undermines the whole point. You start fear-eating carbs “just in case,” which defeats the metabolic benefits.
Reality #3: The most effective dose isn’t always the highest dose you can tolerate. Sometimes 4mg with stable blood sugar beats 8mg with crashes.
Reality #4: This isn’t “just” about weight loss anymore. You’re fundamentally changing how your body processes energy. That requires respect and strategy.
When to Reassess Your Research
Consider pausing or reducing your dose if:
Hypoglycemia events occur more than twice per week
You’re unable to maintain the carbohydrate floor without feeling stuffed
You’re developing anxiety around meal timing
Your activity level or life stress has significantly increased
You’re experiencing sleep disruption from night-time crashes
Remember: the goal of researching these compounds is optimization, not suffering through side effects.
The Bottom Line
Retatrutide represents the cutting edge of metabolic research. That triple-agonist mechanism creates effects we’ve never seen before in this space. But with great power comes great responsibility—and in this case, that responsibility includes managing your carbohydrate intake strategically.
The hypoglycemia issue isn’t a sign that retatrutide “doesn’t work” or that you’re “doing it wrong.” It’s a predictable metabolic consequence of a compound that makes your body incredibly efficient at burning stored energy.
Work WITH your biology, not against it.
And if you found this helpful, share it with someone who needs to read it. The peptide research community works best when we share knowledge openly.
Stay curious. Stay safe. Stay scientific.
—Derek


Again, another balanced and thorough article. I have felt that at times since I went up to 6mg after only two weeks at 4mg... Think I will stick with the 6mg for a while! Almost at my goal anyway, then figuring out maintenance will be my next challenge.
That’s helpful! Could you do some on BPC/TB and Epitalon please? The internet feels random and flooded with all kind of information